Arterite de Takayasu em Paciente Portadora de Síndrome de Down: Relato de Caso
Conteúdo do artigo principal
Resumo
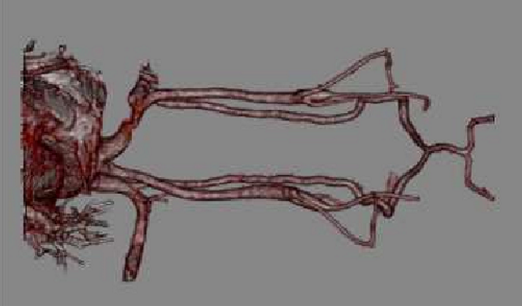
A Arterite de Takayasu é uma vasculite crônica de grandes e médios vasos, que envolve principalmente a aorta e seus ramos proximais. É uma doença incomum que ocorre principalmente em mulheres jovens. À histopatologia, os vasos são caracterizados com infiltrado mononuclear e inflamação granulomatosa da túnica média, levando ao espessamento da parede arterial, com estenose, oclusão e dilatação aneurismática. O presente artigo objetiva apresentar um caso de arterite de Takayasu em uma paciente portadora de Síndrome de Down.
Detalhes do artigo

Este trabalho está licenciado sob uma licença Creative Commons Attribution 4.0 International License.
Authors retain the copyright of their articles and grant the journal the right of first publication under the Creative Commons Attribution (CC BY) license, which allows others to share and adapt the work with proper attribution.
Referências
Noiret B, Renaud F, Piessen G, Eveno C. Multicystic peritoneal mesothelioma: a systematic review of the literature. Pleura Peritoneum. 2019 Sep 1;4(3):20190024. doi: 10.1515/pp-2019-0024.
Gamboa P. Takayasu arteritis. Rev Colomb Cardiol. 2020;27:428-33.
Rodrigues FL. Takayasu arteritis: is age a differential factor in the diagnosis, follow-up, and treatment of the disease? Arq Bras Cardiol. 2023;120(1):e20220877.
Clemente G, Hilário MO, Len C, et al. Brazilian multicenter study of 71 patients with juvenile-onset Takayasu arteritis: clinical and angiographic features. Rev Bras Reumatol Engl Ed. 2016;56(2):145-51.
Coimbra LL, Eduarda M, Leal G, et al. Takayasu arteritis: case report. Braz J Surg Clin Res. 2020;30(3):66-70. Available from: https://www.mastereditora.com.br/periodico/20200508_212706.pdf.
Watanabe R, Berry GJ, Liang DH, Goronzy JJ, Weyand CM. Pathogenesis of giant cell arteritis and Takayasu arteritis: similarities and differences. Curr Rheumatol Rep. 2020;22(10):68.
Aguiar M, Tavares M, Ferreira P, Fernandes F, Nunes G. Clinical case of Takayasu arteritis. In: XVI Seminário Temático em Fisiologia Clínica, ESTeSL; 2023. Available from: https://repositorio.ipl.pt/handle/10400.21/17148
Arend WP, Michel BA, Bloch DA, et al. The American College of Rheumatology 1990 criteria for the classification of Takayasu arteritis. Arthritis Rheum. 1990;33(8):1129-34.
Bhandari S, Butt SRR, Ishfaq A, et al. Pathophysiology, diagnosis, and treatment of Takayasu arteritis: a review of current advances. Cureus. 2023;15(7):e42667.
Renauer PA, Saruhan-Direskeneli G, Coit P, et al. Identification of susceptibility loci in IL6, RPS9/LILRB3, and an intergenic locus on chromosome 21q22 in Takayasu arteritis through a genome-wide association study. Arthritis Rheumatol. 2015;67(5):1361-8.
Panico MDB, Spichler ES, Rodrigues LCD, et al. Takayasu arteritis: clinical and therapeutic aspects in 36 patients. J Vasc Bras. 2008;7(2):123-30.
Duarte MM, Geraldes R, Sousa R, Alarcão J, Costa J. Stroke and transient ischemic attack in Takayasu arteritis: a systematic review and meta-analysis. J Stroke Cerebrovasc Dis. 2016;25(4):781-91.
Grayson PC, Ponte C, Suppiah R, et al. 2022 American College of Rheumatology/EULAR classification criteria for Takayasu arteritis. Ann Rheum Dis. 2022;81(12):1654-60.
Merkel PA, Warrington KJ, Seo P. Clinical features and diagnosis of Takayasu arteritis. In: UpToDate. Waltham (MA): UpToDate; 2023.
Kuroda S, Fujimura M, Takahashi J, et al. Diagnostic criteria for Moyamoya disease – revised version 2021. Neurol Med Chir (Tokyo). 2022;62(7):307-12. Available from: https://www.jstage.jst.go.jp/article/nmc/62/7/62_2022-0072/_article.
Schrager GO, Cohen SJ, Vigman MP. Acute hemiplegia and cortical blindness due to moyamoya disease: a case report in a child with Down syndrome. Pediatrics. 1977;60(1):33-7.
Cramer SC, Robertson RL, Dooling EC, Scott RM. Moyamoya and Down syndrome: clinical and radiological features. Stroke. 1996;27(11):2131-5.
Greene AK, Kim S, Rogers GF, Fishman SJ, Olsen BR, Mulliken JB. Risk of vascular anomalies with Down syndrome. Pediatrics. 2008;121(1):e135-40.
Abdelgadir A, Akram H, Dick MH, et al. A better understanding of moyamoya in trisomy 21: a systematic review. Cureus. 2022;14(3):e23502.
Ren YL, Li TT, Cui W, et al. CD8+ T lymphocyte is a major source of interferon-gamma production in Takayasu arteritis. Sci Rep. 2021;11(1).
Kabeerdoss J, Danda S, Srivastava P, et al. A pilot study of childhood-onset Takayasu arteritis using whole exome sequencing suggests oligogenic inheritance involving classical complement, collagen, and autoinflammatory pathways. Clin Rheumatol. 2024;43(8):2607-13.
Wen D, Feng L, Du X, Dong JZ, Ma CS. Biomarkers in Takayasu arteritis. Int J Cardiol. 2022;371:413-7. Available from: https://www.internationaljournalofcardiology.com/article/S0167-5273(22)01268-2/abstract.
Lee ML, Chang MY, Chang TM, et al. Revascularization of concomitant renal and cerebral artery stenosis in a 14-year-old girl with Takayasu arteritis and Moyamoya syndrome. J Korean Med Sci. 2018;33(10).
Hiraide T, Suzuki H, Momoi M, et al. RNF213-associated vascular disease: a unifying concept of various vasculopathies. Life (Basel). 2022;12(4):555.
Souza AWS, Neves RMS, Oliveira KR, Sato EI. Treatment of Takayasu arteritis. Rev Bras Reumatol. 2006;46(Suppl 1).
Merkel PA, Warrington KJ, Seo P. Treatment of Takayasu arteritis. UpToDate. Available from: https://www.uptodate.com/contents/treatment-of-takayasu-arteritis.
Borelli N. Drug dependence as a disorder or brain disease. Rev Bras Hipertens. 2009;16(4). Available from: http://departamentos.cardiol.br/dha/revista/16-4/16-arterite.pdf.